Pregnancy Loss
You don't have to go through a pregnancy loss alone.
Pregnancy loss doesn't just impact the birthing person. Everyone in the family grieves the loss of a baby.


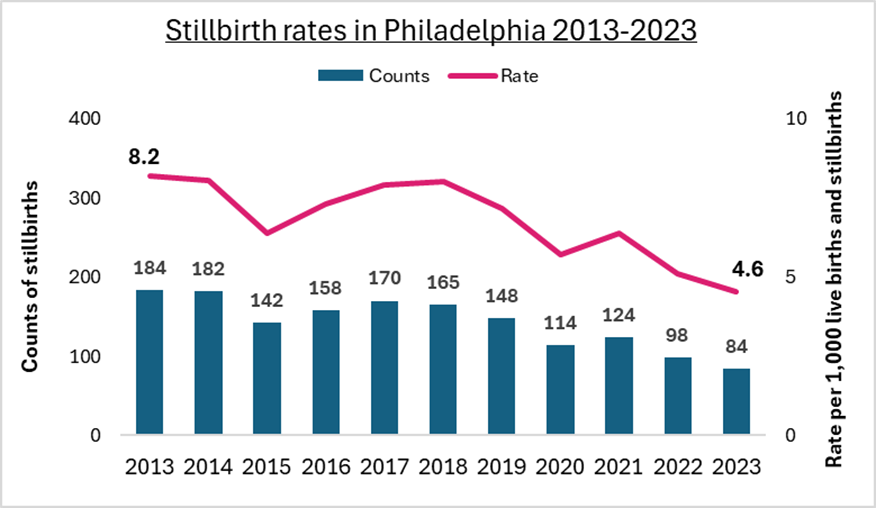
Data source: Pennsylvania Vital Statistics


.jpg)
.jpg)

.jpg)
If you have experienced a miscarriage, stillbirth, or the loss of a baby, your body may still make breast milk, especially if you were 16 weeks or more pregnant. This can be unexpected and emotional.
There is no right or wrong way to respond. What matters most is what feels right for you.
All of this is a normal body response.
You can choose what you want to do about your milk. You can also change your mind at any time. No option is better than another.
You may choose to:
Some people choose to stop milk production. Support may include:

Offers monthly virtual group meetings for persons who have experienced the loss of a pregnancy or infant. Classes are scheduled based on interest.

Offers virtual and text support in English and Spanish. Weekly and monthly phone chat support is available.

Offers in-person and virtual support groups and volunteer opportunities.

Offers free virtual and in-person support groups.

Offers volunteer opportunities, in-person, and virtual support for the birthing person and family members.

Offers support virtual, on-site, or school-based groups for children from aged 4 through high school and virtual support groups for adults.

Offers online support groups which meet weekly or monthly. No pre-registering required.

Offers in-person or virtual counseling services which include individual, intensive outpatient, partial hospitalization, and outpatient programs. Therapists are also available by text for emergency situations.

Offers virtual six-week support groups. Some classes take insurance while others are offered at low-cost.

Offers volunteer opportunities, peer support, and virtual support groups via Facebook.

Offers virtual support groups for all members of the family.

Free virtual support groups and empowerment tools designed specifically for Black parents and caregivers.

Provides financial assistance for burial or cremation services for those who have lost a child. Complete online request for assistance.

Offers helpline staffed by clinicians.

Offers community and peer support insurance assistance and financial assistance towards hospital costs.

Offers individual therapy support, support groups, and referral to additional services.

Offers support groups led by doulas and grief support specialists.

Podcast specifically for men focused on pregnancy and infant loss. Can request one on one conversations with another dad who has experienced loss.

Podcast about going through grief with a mix of personal stories, tips for supporting children, teens, and yourself, and interviews with professionals.

Podcast about pregnancy and infant loss by and for loss parents to share their birth stories of their babies that were stillborn or died in infancy.








Losing a baby at 39 weeks is not something that time, words, or clichés can erase. I carried my baby for almost ten months, felt every movement, planned for their arrival, and imagined our future together. To have all of that end in silence is a grief that reshapes who I am.
What I need from others is compassion without pressure. Please understand that my grief is not something with a quick timeline. It may look different each day sometimes I need to talk about my baby; other times I may need quiet presence. Remembering my child with me, saying their name, and acknowledging important dates like their due date or birthday helps me feel less alone.
I also need people to know that stillbirth is not “just loss.” It is the death of a whole person who was loved, wanted, and expected. My body, my mind, and my heart all went through pregnancy, and then I was left with empty arms. This is a unique kind of grief, mourning the person I never got to raise but loved with my whole being.
What I want people to understand most is that my baby matters. My story and my child’s existence are important. Avoiding the topic or telling me to “move on” does not help. Instead, honoring my baby, allowing me to share my feelings, and offering steady support makes the heaviest days a little lighter.
Stillbirth changes everything. With patience, empathy, and acknowledgment, others can help me carry both my grief and my love forward.
The grief from my loss will always be with me. It has changed and morphed, ebbing and flowing over time. Something will trigger the memory of my infertility and loss, and I'll be right back in those moments. I lost my first child early on, but it didn’t make the experience any less devastating.
I found out I was pregnant after my second intrauterine insemination (IUI) procedure. We had been trying for over two years. It was such a joyous moment, and looking back, I was naive to think that nothing could go wrong. At six weeks, they performed an ultrasound and found nothing but a black void in my uterus. I was told I had to make a decision quickly because the pregnancy was not viable, and keeping it could lead to serious, life-threatening complications for both me and my reproductive system. The next day, I had to undergo a D&C procedure. It was painful and awful, but I’m grateful it saved my reproductive health.
Weeks later, pathology revealed I had experienced a molar pregnancy- a rare condition where cancerous cells grow instead of a healthy pregnancy due to abnormal fertilization. For the next six months, I had to be closely monitored by an oncology team to ensure no cancer cells remained. We were told we couldn’t try again during this time, which felt like a huge blow to our infertility journey. I felt isolated and alone, no one who truly understood my experience. Thankfully, cancer never developed, and I was eventually cleared to try again.
Soon after, I became pregnant naturally, without fertility treatments. Deep down, I knew something was happening, but I was in denial until I took a test to confirm. The clinic confirmed the pregnancy, but it ended in a missed miscarriage. Two losses in six months – it felt like an endless cycle of grief and heartbreak. It was so hard to believe I’d ever feel anything but pain from fertility.
Three months later, I decided to try IUI one last time, with IVF as our next step if it didn’t work. In September, we went through with the procedure, and it was successful. But pregnancy after loss brought overwhelming anxiety; joy was hard to find. I felt jaded, my excitement was dulled by fear and painful memories.
My grief over those two losses kept me from fully embracing this new pregnancy. But as the weeks went on, I graduated from my fertility clinic and transitioned to an OBGYN. Things continued to go well, and our baby was growing strong. In June 2025, I gave birth to a healthy baby. On sleepless nights, I sometimes tell her the story of our fertility journey and how it led to her. Sharing helps me process the grief I still carry. I remember my first loss vividly and the pain that came with it. The pain hasn’t disappeared, but it has softened.
Certain songs still bring me to tear, taking me back to that period of that grief and sorrow. Yet I’m deeply grateful for where I am today, holding my beautiful baby girl. Knowing the challenges we overcame to have her make her presence eve
To honor my first loss, I wear a miscarriage ring representing the size of the baby when I lost my first pregnancy. I wear it every day.

When I found out I was pregnant for the third time, I was thrilled. I kept the news a surprise from my 6-year-old daughter because she had been asking for a sibling. She prayed every night for a baby sister but told me she would be happy as long as the baby was healthy. When I finally shared the news with her, she was overjoyed.
I scheduled my prenatal care and prepared for my first ultrasound. I was excited to hear the heartbeat, and I brought both my children– my 6-year-old and my 18-year-old so they could share in the joy. That very morning, I had a vivid dream of seeing a fetus on an ultrasound screen. In the dream, it rose, wobbled up twelve steps, and disappeared. I thought it was a sign that everything was okay.
At the appointment, the technician began the scan in silence. The room felt heavy. After a few passes, I whispered, “Not good news.” He explained that only the doctor would confirm. In that moment, I knew.
The doctor came in and confirmed that there was no heartbeat. I think I went into shock. I tried to comfort myself with thoughts like “It’s God’s will” and “God knows better”. While I wanted toaccept that, my heart and my mind were conflicted.
It took about two weeks for my body to pass the baby. I was 3-4 months along. I labored at home and delivered the fetus still in the amniotic sac. The physical pain was constant, but the emotional pain cut even deeper. For me, the loss was harder than either of my full-term labors. I buried my baby on family land, near a tree. That tree has become a place of connection. I still cry sometimes, but I also honor my child there. I hug the tree, I sit with it, and I believe my baby’s spirit watches over us as a guardian angel. My daughter, now 7, still prays for sibling and speaks to the clouds, keeping the bond alive in her own way.
I plan to decorate the tree with flowers and create a memorial garden. I will place a chair nearby where I can sit and talk, and eventually a memorial marker with a name. I believe energy cannot be created nor destroyed. My child’s time with me was brief, but their presence was real. Though the life may have felt incomplete to me, it was complete in what was meant to be. I honor my baby by remembering, by loving, and by creating a space where their energy continues to live.

Provides free to print and bulk order brochures, bookmarks, and rack cards
Type of support: Patient Materials

Bedside bereavement program in-hospital [call/text: 856-656-6346]
Perinatal bereavement training for providers and volunteers who support parents of loss
Type of support: Training, Bereavement Care In-Hospital
.svg)
Remembrance carts for hospitals, healthcare bereavement training via video or in-person for staff
Type of support: Patient Materials, Training

Online bereavement training, memory making workshop to learn how to honor the life lost
Type of support: Training
.svg)
Latest research information, virtual or in-person training with continuing education credits, free patient brochures
Type of support: Education, Training, Patient Materials, CE Credits

Perinatal bereavement and trauma-informed training with CE credits offered.
Type of support: Training, CE Credits

Stillbirth toolkit, international standards of practice, virtual training, bereavement-related research articles
Type of support: Education, Training, Patient Materials

Virtual and on-demand training with CE credits
Type of support: Patient Materials

IMPROVE-USA half-day perinatal bereavement training
Type of support: Training, CE Credits

Perinatal Bereavement Certificate Program, resources for cultural and religious bereavement rituals, photography and communication tips, etc.
Type of support: Training, Resources, CE Credits

Perinatal bereavement photography training
Type of support: Training, CE Credits
Evidence-based, best practices for perinatal providers
From the National Health Service, England
From the Centre of Research Excellence Stillbirth, Australia



.jpg)







